EARLIEST DESCRIPTIONS OF SYMPTOMS DEFINING IBS
- 1849 – W Cumming1“The bowels are at one time constipated,at another lax, in the same person. How the disease has two such different symptoms I do not profess to explain. . . .”
- Other historical terms – mucous colitis – colonic spasm – neurogenic mucous colitis – irritable colon – unstable colon – nervous colon – spastic colon – nervous colitis – spastic colitis1962 – Chaudhary & Truelove2 Irritable colon syndrome1966 – CJ DeLor3 Irritable bowel syndrome
HISTORICAL PERSPECTIVE
sufferers are women)2– condition not fatal
•Long dismissed as a psychosomatic condition1 no clear etiology– affects predominantly women(~70% of
•Attitudes now changing
•Incidence and prevalence not extensively monitored in past
HALLMARK SYMPTOMS OF IBS
•Chronic or recurrent GI symptoms– lower abdominal pain/discomfort– altered bowel function (urgency,altered stool consistency, altered stool frequency, incomplete evacuation)– bloating
•Not explained by identifiable structural or
biochemical abnormalities
KEY FACTS ABOUT IBS
- Up to 20% of the US population report symptoms consistent with IBS1
- The most common GI diagnosis among gastroenterology practices in the US2
- One of the top 10 reasons for PCP visits3
- Affects predominantly females (~70% of sufferers)4
- The most common functional bowel disorder5
- Can cause great discomfort, sometimes intermittent or continuous, for many decades in a patient’s life1
- Can significantly disrupt daily life2
- Can have negative impact on quality of life2
- Current treatment options– dietary modification– fiber supplements– pharmacologic agents– psychotherapy
- Success of current treatment options in addressing multiple symptoms of IBS has been limited4
iBS Consultation pattern
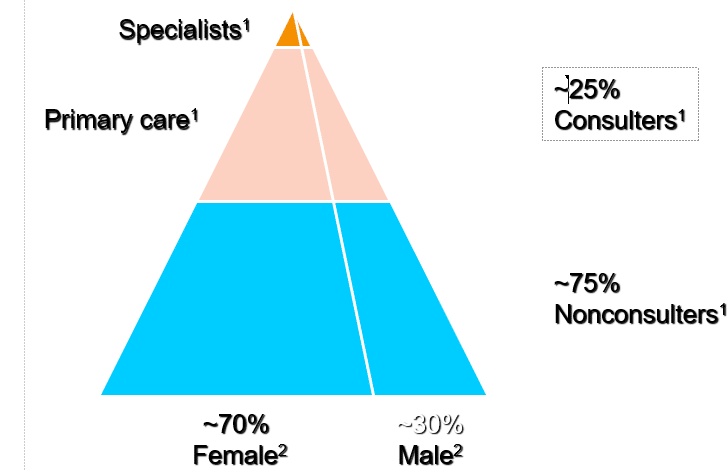
DIRECT MEDICAL COSTS ASSOCIATED WITH IBS
- BS results in an estimated $8 billion in direct medical costs annually1
- IBS sufferers incur 74% more direct healthcare costs than non-IBS sufferers1
- IBS patients have more physician visits for both GI and non-GI complaints2
PRODUCTIVITY BURDEN
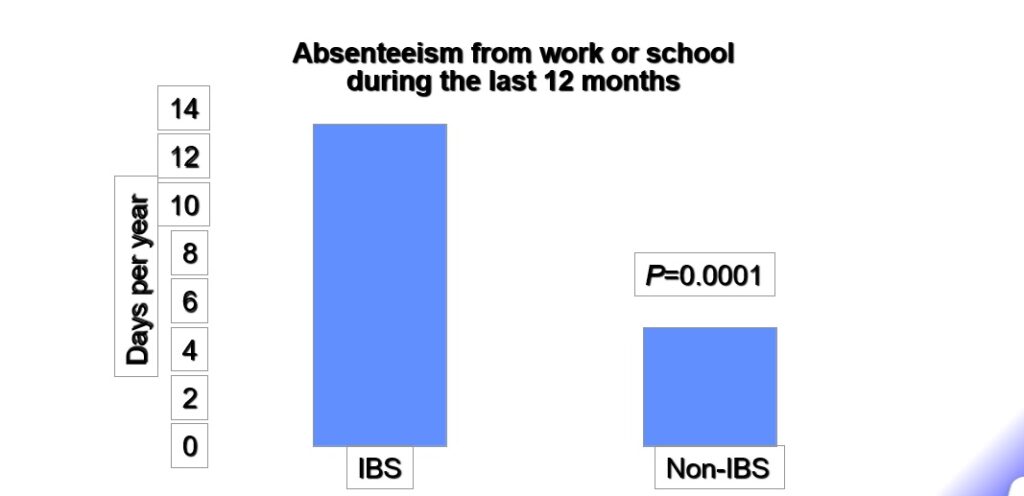
Impact on work due to IBS
Patients with some missed workdays — 30%
Average number missed workdays* — 1.7
Patients who cut back some days — 46%
Average number days cut back* — 3
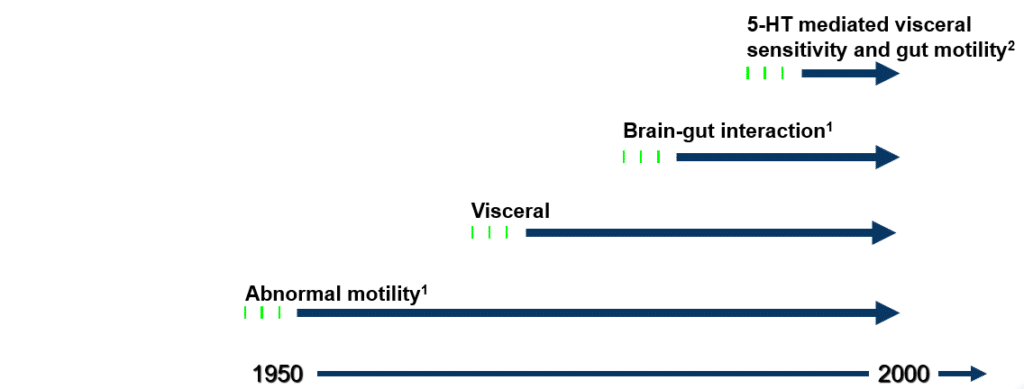
EVOLUTION OF MECHANISTIC HYPOTHESES IN IBS
IRRITABLE BOWEL SYNDROME
- Biopsychosocial Disorder–Psychosocial–Motility–Sensory–? Infectious
- Prevalence 10%, Incidence 1-2% per Year
- Disturbs QOL, Social Function, Healthcare Utilization
ENTERIC NERVOUS SYSTEM
- Controls motility and secretory functions of the intestine
- Semiautonomous– actions modified by parasympathetic and sympathetic nervous systems– may function independently
- Contains many neurotransmitters, including 5-HT, substance P, VIP (vasoactive intestinal peptide), and CGRP (calcitonin gene-related peptide)
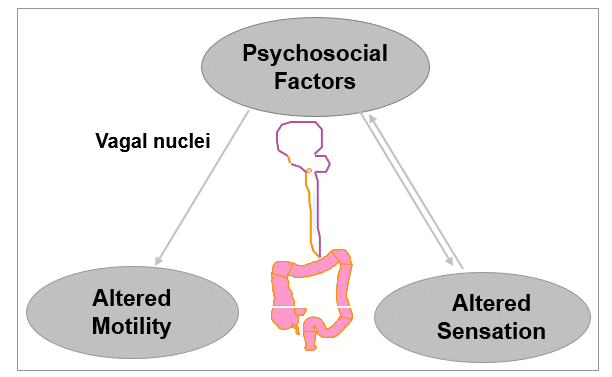
IBS: Current thinking on pathophysiology
Defects in the enteric nervous system may leadto the hallmark symptoms of IBS
- Visceral hypersensitivity1 – Increased visceral afferent response to normal as well as noxious stimuli– Mediators include 5-HT, bradykinin, tachykinins, CGRP, and neurotropins
- Primary motility disorder of GI tract2 – Mediated by 5-HT, acetylcholine, ATP, motilin, nitric oxide, somatostatin, substance P, and VIP
PHYSIOLOGICAL DISTRIBUTION OF 5-HT
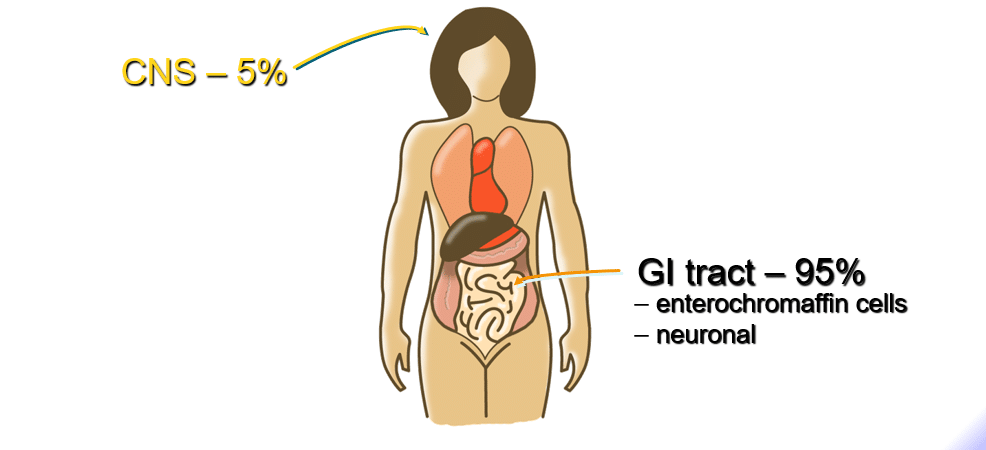
5-HT initiates peristaltic reflex mediated by the ENS
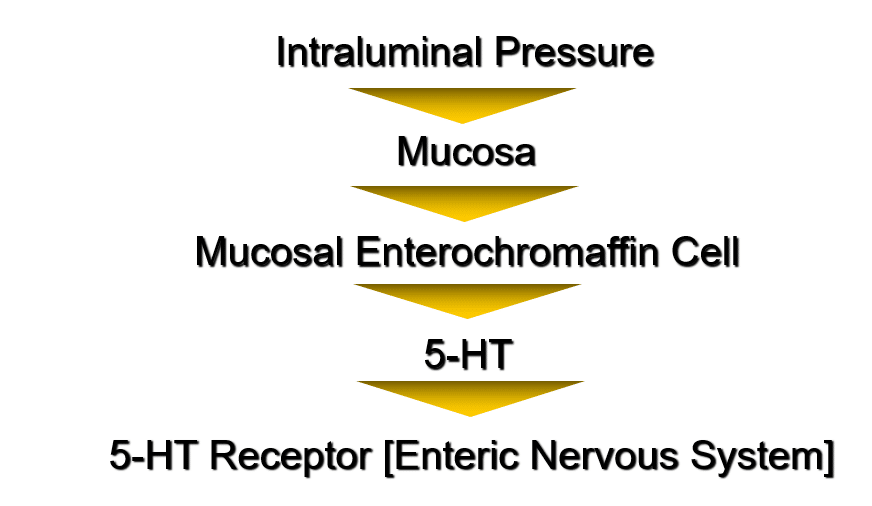
5-HT RECEPTOR EFFECTS
- •Mediate reflexes controlling gastrointestinal motility and secretion
- Mediate perception of visceral pain
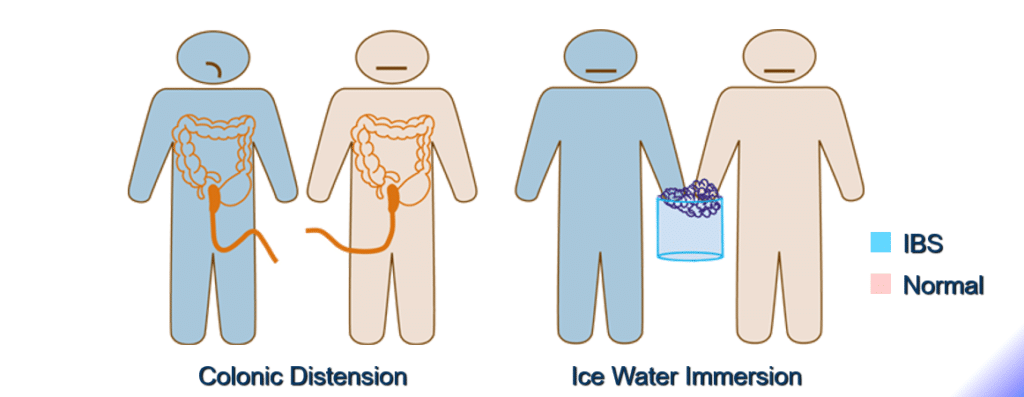
COMPARISON OF PAIN THRESHOLDS OF IBS PATIENTS AND CONTROLS
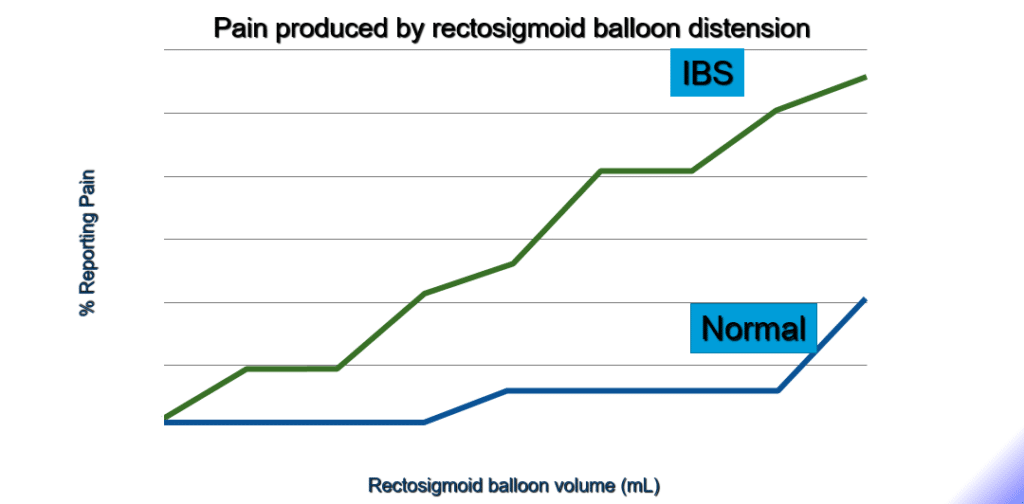
COMPARISON OF PAIN THRESHOLDS
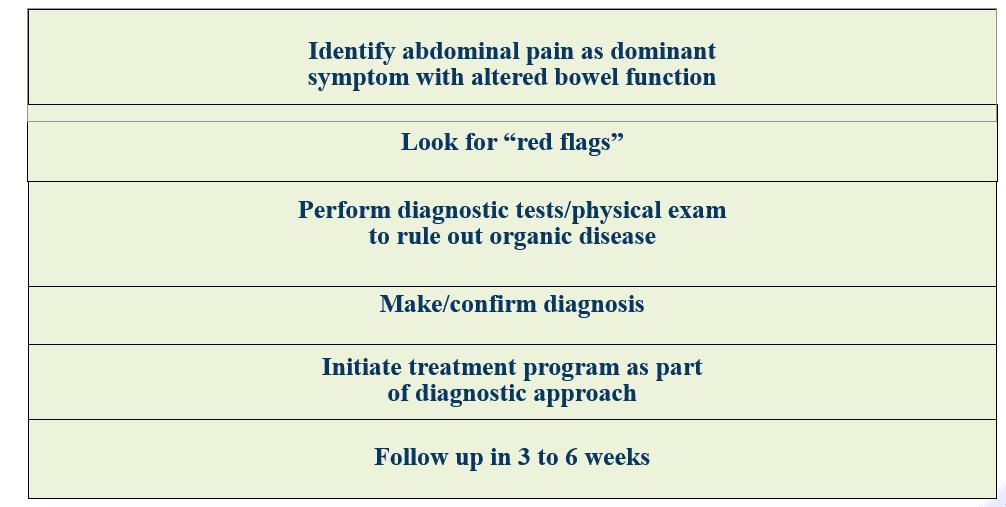
MAKE A POSITIVE DIAGNOSIS1,2
HISTORY OF DIAGNOSTIC APPROACHES
- 1950s – Increased gut motility1
- 1970s – Specific motility markers1
- 1980 to 1999 – Symptom-based criteria1–Manning criteria–Rome criteria
- 1999 – Rome II criteria2
IBS ROME II CRITERIA
At Least 12 Weeks, Which Need Not Be Consecutive, in the Preceding 12 Months, of Abdominal Discomfort or Pain That Has Two of Three Features:
1.Relieved with Defecation; and/or
2. Onset Associated with a Change in Frequency of Stool; and/or
3. Onset Associated with a Change in Form (Appearance) of Stool
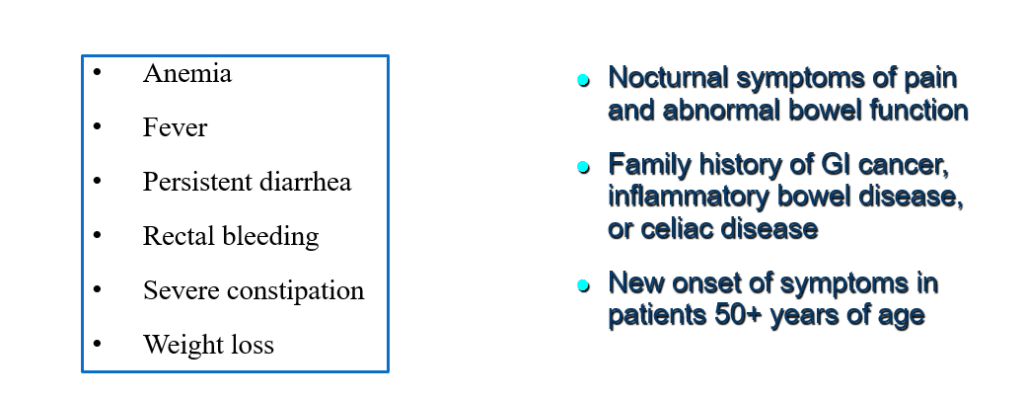
RED FLAGS” MAY SUGGEST AN ALTERNATIVE OR COEXISTING DIAGNOSIS

DIAGNOSTIC TESTS—WHAT? WHEN? WHO?
If patient has typical features of IBS:
•If <50 years of age, order CBC, electrolytes, LFTs, screen stool for occult blood, and consider sigmoidoscopy.1
•If ³50 years of age, order CBC, electrolytes, LFTs, and perform a colonoscopy or air-contrast barium enema with sigmoidoscopy.1,2
DIFFERENTIAL DIAGNOSIS
- Malabsorption1
- Dietary factors1
- Infection1
- Inflammatory bowel disease1
- Psychological disorders1
- Gynecological disorders2
- Miscellaneous1
CURRENT MANAGEMENT OF IBS
- Establish a positive diagnosis1
- Reassure patient that there is no serious
organic disease or alarming symptoms1 - Success of current treatment options in addressing multiple symptoms of IBS has been limited2
CURRENT MANAGEMENT COMPONENTS OF IBS
- Education
- Reassurance•Dietary modification
- Fiber
- Symptomatic treatment
- Psychological/behavioral options
- Realistic goals
Laxatives and bulking agents
Symptomatic treatment—constipation
- Increased dietary fiber or psyllium1
- Osmotic laxatives (MgSO4, lactulose)2
- Stimulant laxatives3
- Some laxatives and bulking agents can exacerbate abdominal pain and bloating3
TRICYCLIC ANTIDEPRESSANTS AND SSRIS
Symptomatic treatment—pain
•Reserved for patients with severe or refractory pain
Multiple medications needed to treat multiple symptoms
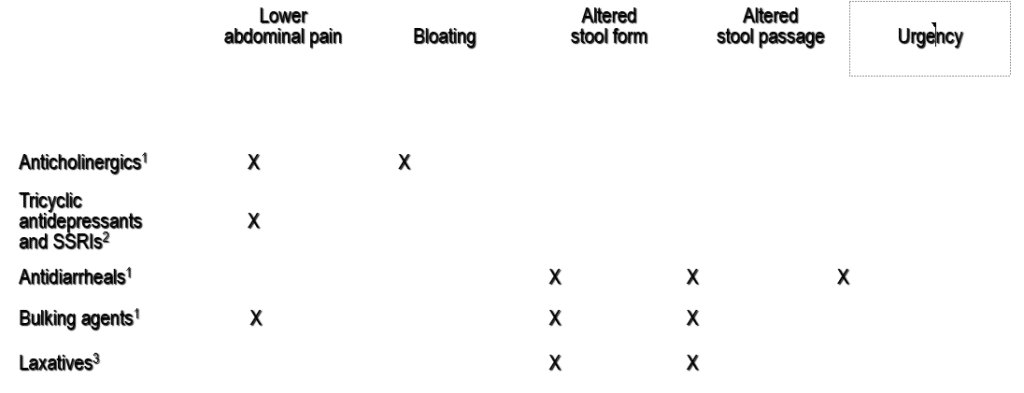
A COMPREHENSIVE MULTICOMPONENT APPROACH
Treatment program is based on dominant symptoms and their severity and on psychosocial factors
- Medical management
- Diet
- Psychological or behavioral options– psychotherapy– stress management
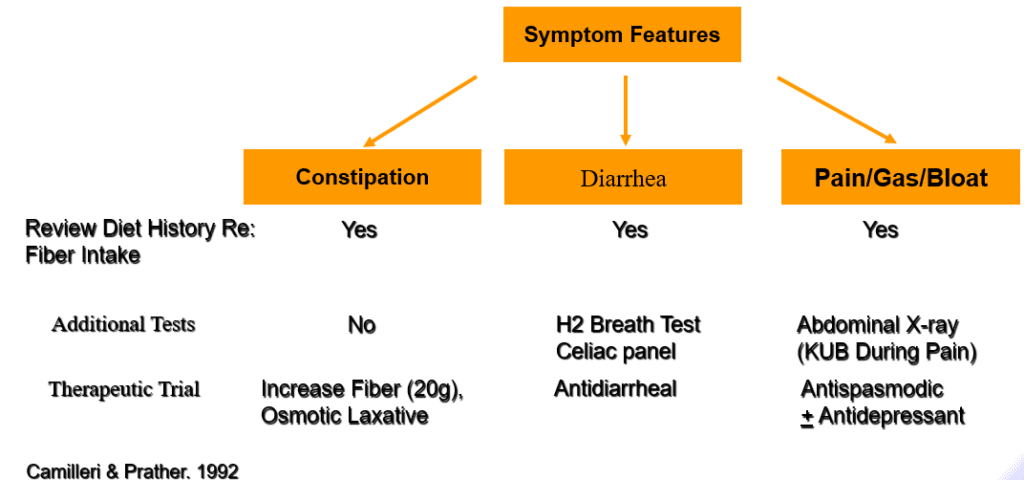
INITIAL MANAGEMENT OF IBS
Non-Traditional Remedies
- Chinese Herbal Medicine –116 pts randomized to CHM did better than pts receiving placebo
- Peppermint Oil–Relaxation of GI smooth muscle–Meta-analysis showed significant improvement of IBS symptoms
- Acupunture
- Probiotics
- Antibiotics
Surgical Therapy for IBS
- IBS symptoms may be attributed to:–Non-functioning gallbladder disease, chronic appendicitis, uterine fibroids, tortuous colon
- IBS symptoms rarely improve after surgery
- IBS patients 2 to 3 times more likely to undergo unnecessary surgery
Take Home Points
•IBS is a chronic medical condition characterized by abdominal pain, diarrhea or constipation, bloating, passage of mucus and feelings of incomplete evacuation
•Precise etiology of IBS is unknown and therefore treatment is focused on relieving symptoms rather that “curing disease”
Take Home Points
- Although many IBS patients complain of symptoms after eating, true food allergies are uncommon
- Specific therapies are determined by individual patient symptoms
- Life-style modifications and possible alternative therapies may relieve symptoms
- Surgery has NO Role in treatment of IBS